Day 3 :
Keynote Forum
Igor I. Tulevski
Cardiologie Centra Nederland, The Netherlands
Keynote: The Future is in the clicks and not in the Bricks, how to cope with the incresaing demand
Time : 09:30-10:00

Biography:
Igor Tulevski is a cardiologist and co-founder of CCN. In addition to cardiology, his subspecialism is congenital cardiology, imaging and sports cardiology, right chamber overload, congenital heart defects in adults. He is also Chairman of the Supervisory Board of De Sionsberg Hospital in Dokkum and is active in various working groups such as NVVC Work Group Nuclear Imaging, MRI and CT, Pulmonary Circulation and Right Ventricular Function of the European Society of Cardiology and member of the European Society of Cardiology (FESC).
Abstract:
- Sessions
Location: Amsterdam, Netherlands
Session Introduction
Faezeh Sahbaeiroy
Iran
Title: Differences between current clinical and American Heart Association blood pressure measurement techniques
Time : 10:10-10:40
Biography:
Abstract:
Statement of the Problem: The guidelines recommended by American Heart Association for blood pressure measurement are commonly by health workers who take blood pressure .For taking blood pressure ,it is important to apply standard methods. If we do it with a few mistakes the result may be effect in patient's medication.
The purpose of this study: Is to compare the rate and accuracy of measuring blood pressure by Health Workers methods and American Heart Association Technique.
Methodology: For validation of this observation we designed a descriptive and observational study to be carried out in seven hospitals. Four hundred health workers divided into four groups (125 nurses 100 nursing students 100 medical students 75 physicians) were evaluated in a two part test. In first part (practical) the examinee had to follow all steps recommended by American Heart Association to get a passing score. In the second part (theoretical which came second to avoid influencing the practical) the examinee had to answer correctly 8 questions based on American Heart Association's guidelines to obtain a passing score.
Findings: 52.5 % of systolic and 49.3% of diastolic readings was out of range. Nursing students obtained the best practical results (52% systolic and 39% diastolic within range) and physicians obtained the lowest values (18.5% and 31.4%). These two groups showed deficiencies in the theoretical test (physicians 7.6% correct answers and Nursing students 19.5%). Medical students obtained the best results on the theoretical test (73% correct P<0.001 versus the other groups) but were deficient in the practical test (28% systolic and 42% diastolic within range).
Conclusion: In conclusion health workers used various techniques for measurement and no completely followed the standard. Such measurements may affect diagnosis and treatment of hypertension but measuring all BPs solely by the standard is not practical. We need to have a practical and efficient method for measuring BP.
References:
- Burgess SE, MacLaughlin EJ, Smith PA, Salcido A, Benton TJ.(2011) Blood pressure rising: differences between current clinical and recommended measurement techniques. J Am Soc Hypertens., 5:484–488.
- Piper MA, Evans CV, Burda BU, et al., (2015) Diagnostic and predictive accuracy of blood pressure screening methods with consideration of rescreening intervals: a systematic review for the U.S. Preventive Services Task Force. Ann Intern Med; 162:192.
- Bakris GL. (2016) The Implications of Blood Pressure Measurement Methods on Treatment Targets for Blood Pressure. Circulation; 134:904.
- Powers BJ, Olsen MK, Smith VA, et al., (2011) Measuring blood pressure for decision making and quality reporting: where and how many measures? Ann Intern Med; 154:781
- Lamarre-Cliché M, Cheong NN, Larochelle P. (2011) Comparative assessment of four blood pressure measurement methods in hypertensives. Can J Cardiol: 27: 455.
Bum Ju Lee
Korea Institute of Oriental Medicine, KR
Title: Prediction of pre-hypertension and metabolic syndrome using combined obesity indices based on machine learning
Time : 11:00-11:30

Biography:
Bum Ju Lee has his expertise in evaluation in association between anthropometric indices and metabolic abnormalities. He studied the relationship between anthropometric indices related to obesity and hypertension, hypotension, type 2 diabetes, hypertriglyceridemia, and serum high- and low-density lipoproteins, and have published many articles with these contents. He is currently a senior researcher in the Korea Institute of Oriental Medicine, Daejeon, Korea. His research interests include data mining and database, bioinformatics, public health, epidemiology, and oriental medicine. Funding: NRF-2006-2005173, NRF-2012-0009830, NRF- 2009-0090900, and NRF-2015M3A9B6027139. BJL: corresponding author.
Abstract:
Statement of the Problem: Hypertension and metabolic syndrome (MetS) are a common health problem. Many previous studies reported that MetS and hypertension were strongly associated with obesity. However, no studies on the prediction of pre-hypertension and MetS using combined anthropometric indices related to obesity have been reported. The objectives of this study were to predict pre-hypertension and MetS using combined anthropometric indices based on machine learning and to evaluate the quality of various predictive models.
Methodology & Theoretical Orientation: A total of 3,927 subjects aged 40-70 years participated in this study. To diagnose pre-hypertension and MetS, we considered the recommendations of the National Cholesterol Education Program Adult Treatment Panel III. For anthropometric indices, eight circumferences (forehead, neck, axilla, chest, rib, waist, pelvis, and hip) were measured. We calculated the ratios between the indices. Finally, we extracted a total of 41 variables including age, weight, height, waist-to-hip ratio, waist-to-height ratio, body mass index, neck-to-rib ratio, and so on. For model building, correlation-based feature selection and wrapper-based variable selection based on logistic regression (LR) and naïve Bayes (NB) were used to identify the optimal variable subsets.
Findings: There were 1,605 men with pre-hypertension (41%) and 1,136 (29%) with MetS. We tested six models in each disease (Figure 1). The LR-wrapper model showed the highest predictive power. The ROC values for the pre-hypertension and MetS were 0.645 and 0.819, respectively. In MetS, the model using combined indices showed slight improvements in the ROC compared with the waist circumference (ROC = 0.809 by NB and LR), even though waist circumference is one of the five components used to diagnose MetS and is a strong predictor of MetS.
Conclusion & Significance: Our results provide insight into a simple and inexpensive method that could be used to identify pre-hypertension and MetS in initial health screening.
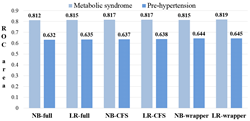
Figure 1: Predictive power of metabolic syndrome and pre-hypertension using combined anthropometric indices (NB: naïve Bayes, LR: logistic regression, CFS: correlation-based feature selection method, wrapper: wrapper-based feature selection method, ROC: the receiver operating characteristic curve)
References:
- Lee BJ, Kim JY (2014) A comparison of the predictive power of anthropometric indices for hypertension and hypotension risk. PLoS One 9:e84897.
- Asayama K, Sato A, Ohkubo T, et al. (2009) The association between masked hypertension and waist circumference as an obesity-related anthropometric index for metabolic syndrome: the Ohasama study. Hypertens Res 32:438-443.
- Lee BJ, Ku B, Nam J, et al. (2014) Prediction of fasting plasma glucose status using anthropometric measures for diagnosing type 2 diabetes. IEEE J Biomed Health Inform 18:555-561.
- Lee BJ, Nam J, Kim JY (2016) Predictors of metabolic abnormalities in phenotypes that combined anthropometric indices and triglycerides. BMC Complement Altern Med 16:59.
- Lee BJ, Kim JY (2016) Identification of Type 2 Diabetes Risk Factors Using Phenotypes Consisting of Anthropometry and Triglycerides based on Machine Learning. IEEE J Biomed Health Inform 20:39-46
Haben Tsehaye Ghebray
Mekane Hiwet Medical Center, Uganda
Title: Myocardial perfusion scan; a case study
Time : 11:30-12:00

Biography:
Haben Tsehaye is a medical doctor who has been practising in internal medicine and cardiology for the last 6 years. He holds his degrees from Orotta School of medicine. He is very vigilant and hardworking. He has worked in different hospitals. His passion for cardiology has enabled him to work more on this field and take care of patients with cardiac diseases. He has presented many cardiology and internal medicine cases in different occasions. His interest in publishing and research is enormous.
Abstract:
Coronary artery disease remains major health concern and leading cause of death throughout the world. Effective assessment with non-invasive test such as myocardial perfusion scan, exercise stress test and stress echocardiography with dobutamine can provide useful diagnostic and prognostic information. Here we discuss the role of myocardial perfusion scan in 55 year old hypertensive diabetic and obese patient with exertional chest pain and shortness of breath. His baseline ECG was normal with some nonspecific ST-T changes and ECHO with EF OF 50% and no structural or regional motion wall abnormality. Patient was tried with exercise test but because of dyspnea and his obesity will hinder the echocardiography window, we stopped exercise and dobutamine echocardiography test and decided adenosine myocardial perfusion scan. The MPS scan result showed reversible ischemia in anterioseptoapical portion of the myocardium and then angiography was done and showed 90% stenosis in the mid LAD. Patient was stented with DES and started on dual antiplatelet and imporved clinically and he is doing good on his follow up and no complaint of dypnea or exertional chest pain.
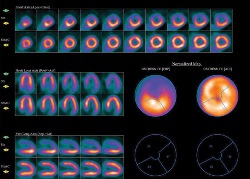
Figure1: The result of the MPS as seen above.
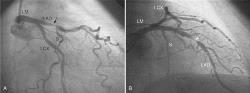
Figure 2: Angiography result of mid lad stenosis.
References:
- Santos-Ocampo C D, Herman S D and Travin M I, et al. (1994) Comparison of exercise, dipyridamole, and adenosine by use of technetium 99m sestamibi tomographic imaging. Journal of Nuclear Cardiology 1:57–64.
- Henzlova M J, Cerqueira M D, Hansen C L, Taillefer R and Yao S S (2009) ASNC Announcement. Journal of Nuclear Cardiology 16:331.
- Marzilli M, Merz C N and Boden W E, et al (2012) Obstructive coronary atherosclerosis and ischemic heart disease: an elusive link. Journal of the American College of Cardiology 60:951–56.
- Hachamovitch R, Hayes S and Friedman J D, et al. (2003) Determinants of risk and its temporal variation in patients with normal stress myocardial perfusion scans: what is the warranty period of a normal scan, Journal of the American College of Cardiology 41:1329–40.
- Zoghbi G J, Dorfman T A and Iskandrian A E (2008) The effects of medications on myocardial perfusion. Journal of the American College of Cardiology 52:401–16.
A.J. van Ballegooijen
VU University, Amsterdam, the Netherlands
Title: The joint association of vitamin D and vitamin K with incident hypertension and cardiovascular health
Biography:
Hanne van Ballegooijen, is a nutritional-epidemiologist who is currently working at the VU University. Her main expertise is in the field of mineral metabolism disturbances and cardiovascular disease risk. After her PhD she received a personal grant (2013) to work at the Kidney Research Institute at the University of Washington, Seattle in the group of Jonathan Himmelfarb and Bryan Kestenbaum and studied nutritional determinants in chronic kidney patients. Her research interests include nutrition and lifestyle determinants in the etiology of chronic diseases. She has a particular interest in how mineral metabolism disturbances affect cardiovascular disease risk. A better understanding of these relationships may help to promote cardiovascular health.
Abstract:
Statement of the Problem: Cardiovascular disease and osteoporosis are major age-related causes of morbidity and premature death that occur among older adults. Emerging evidence suggests that calcium from bone is deposited in the arteries. This leads to calcification in valves and vessels, which is associated with a 3-4 fold higher risk of coronary heart disease. Calcium and vitamin D supplementation is frequently advised in older adults for the prevention of osteoporosis and to reduce the risk of fractures and falls. However, recent RCT's showed that individuals taking calcium and vitamin D were at higher risk of cardiovascular disease. The widespread use of vitamin D and calcium supplements, and the fortification of vitamin D in food products, underscores the need for further investigation.
Recent studies show that vitamin K reduces coronary calcification and cardiovascular disease. New evidence suggests that vitamin K combined with vitamin D can lower vascular calcification more than the effect of either alone. This presentation will give a brief overview of the current body of evidence of joint associations between vitamin D and vitamin K with hypertension and underlying mechanisms of cardiovascular disease in multiple cohort studies.
Conclusion & significance: The combination of low vitamin D and K status is associated with increased blood pressure and might play a role in development of hypertension and cardiovascular disease risk. These promising results of the joint associations of vitamin D and vitamin K in relation to cardiovascular health stimulate further follow-up studies to better understand the clinical implications of this relationship to promote cardiovascular health.
A.J. van Ballegooijen
VU University, Amsterdam, the Netherlands
Title: The joint association of vitamin D and vitamin K with incident hypertension and cardiovascular health
Time : 12:00-12:30

Biography:
Hanne van Ballegooijen, is a nutritional-epidemiologist who is currently working at the VU University. Her main expertise is in the field of mineral metabolism disturbances and cardiovascular disease risk. After her PhD she received a personal grant (2013) to work at the Kidney Research Institute at the University of Washington, Seattle in the group of Jonathan Himmelfarb and Bryan Kestenbaum and studied nutritional determinants in chronic kidney patients. Her research interests include nutrition and lifestyle determinants in the etiology of chronic diseases. She has a particular interest in how mineral metabolism disturbances affect cardiovascular disease risk. A better understanding of these relationships may help to promote cardiovascular health.
Abstract:
Statement of the Problem: Cardiovascular disease and osteoporosis are major age-related causes of morbidity and premature death that occur among older adults. Emerging evidence suggests that calcium from bone is deposited in the arteries. This leads to calcification in valves and vessels, which is associated with a 3-4 fold higher risk of coronary heart disease. Calcium and vitamin D supplementation is frequently advised in older adults for the prevention of osteoporosis and to reduce the risk of fractures and falls. However, recent RCT's showed that individuals taking calcium and vitamin D were at higher risk of cardiovascular disease. The widespread use of vitamin D and calcium supplements, and the fortification of vitamin D in food products, underscores the need for further investigation.
Recent studies show that vitamin K reduces coronary calcification and cardiovascular disease. New evidence suggests that vitamin K combined with vitamin D can lower vascular calcification more than the effect of either alone. This presentation will give a brief overview of the current body of evidence of joint associations between vitamin D and vitamin K with hypertension and underlying mechanisms of cardiovascular disease in multiple cohort studies.
Conclusion & significance: The combination of low vitamin D and K status is associated with increased blood pressure and might play a role in development of hypertension and cardiovascular disease risk. These promising results of the joint associations of vitamin D and vitamin K in relation to cardiovascular health stimulate further follow-up studies to better understand the clinical implications of this relationship to promote cardiovascular health.
References:
- Van Ballegooijen AJ, Rhee EP, Elmariah S, de Boer IH, Kestenbaum B., (2015), Renal Clearance of Mineral Metabolism Biomarkers. J Am Soc Nephrol, ASN 2014, 21253.
- Van Ballegooijen, AJ, Gansevoort, RT, Lambers-Heerspink H, de Zeeuw D, Visser M, Brouwer IA, Kema IP, de Borst MH, Bakker SJ, Joosten MM.(2015), Plasma 1, 25-Dihydroxyvitamin D and the Risk of Developing Hypertension, the Prevention of Renal and Vascular End-Stage Disease Study. Hypertension; 66(3):563-70.
- Van Ballegooijen AJ, Kestenbaum B, Sachs MC, de Boer IH, et al.,(2014), Association of 25-hydroxyvitamin D and Parathyroid Hormone with Incident Hypertension: The Multi-Ethnic Study of Atherosclerosis J Am Coll Cardiol.; S0735-1097(14)00300-3.
- Van Ballegooijen AJ, Visser M, Cothc MF, Arai AE, et al., (2013) Serum Vitamin D and Parathyroid Hormone in Relation to Cardiac Structure and Function: the ICELAND-MI Substudy of AGES-Reykjavik. J Clin Endocrinol Metab.; 98: 2544-2552.
- Van Ballegooijen AJ, Reinders I, Visser M, Brouwer IA., (2013), Parathyroid hormone and cardiovascular disease events: A systematic review and meta-analysis of prospective studies, Am Heart J.; 165(5):655-64, 664.e1-5.
Fatemeh Esfarjani
Shahid Beheshti University of Medical Sciences, Iran
Title: Metabolic syndrome and blood pressure, predict cardio vascular risk factors
Time : 12:30-13:00

Biography:
Fatemeh Esfarjani is a academic member of food and nutrition policy and planing research department, in national nutrition and food technology research institute , she has years of experience in research, evaluation, teaching and administration both in hospital and education institutions. Her field of interest is in clinical nutrition, she published 23 papers in academic journals and more than 124 abstract presentations in congresses.
Abstract:
Childhood obesity increases the risk of metabolic syndrome (MetS) both in childhood and adulthood. The present study was determined the prevalence of MetS and its potential determinants in a representative sample of obese children. This cross-sectional study was conducted among 150 obese children. body mass index (BMI≥95th percentile) with seven years of age. They were randomly selected from 9 health centers in 3 districts of the north Tehran. Trained nutritionists completed a socio-demographic questionnaire by interviewing parents, and conducted the physical examination. Mets was defined based on modified ATP III criteria. The mean (SD) of weight, height, and BMI was 37.5 (6.3) kg, 127.2 (4.7) cm and 23.08 (2.9) kg/m2, respectively. The prevalence of MetS was 13.4%, without significant difference in terms of gender. The most common component of MetS was abdominal obesity (79%). While 21.3% of children did not have any component of MetS, 42% of them had at least one component. Most children with MetS had a history of breastfeeding for less than 6 months. Waist circumference, systolic and diastolic blood pressure, fasting blood glucose, and triglyceride levels were higher in Mets compared to controls (p<0.05). Logistic regression model revealed that children with birth weight of ≤2500 gr. were at higher risk of MetS than children with a higher birth weight (OR=4.3; 95%CI: 1.1-9.7). Primordial prevention of childhood obesity, screening the components of MetS among obese children and assessing the clustering of risk factors is associated with an increased risk of cardiovascular disease. Therefore, these components should be considered as a health priority at individual and public levels.
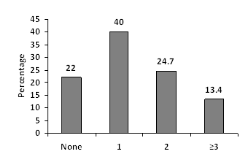
Figure 1: Frequency of obese children according to the number of metabolic syndrome components.
References:
- Kelishadi R. (2007) Childhood overweight, obesity, and the metabolic syndrome in developing countries, Epidemiologic reviews, 29 (1): 62-76.
- Karnik S, Kanekar AS., (2011) Childhood Obesity: A Global Public Health Crisis, International Journal of Preventive Medicine, 3(1).
- Sen Y, Kandemir N, Alikasifoglu A, Gonc N, Ozon A., ( 2008), Prevalence and risk factors of metabolic syndrome in obese children and adolescents: the role of the severity of obesity. European journal of pediatrics, 2008, 167(10): 1183-9.
- Esfarjani F. (2012) Assessing the effect of lifestyle modification intervention in school-age obese Children. Final Report National Nutrition and Food Technology Research Institute. Tehran, Iran.
- Barzin M, Hosseinpanah F, Saber H, Sarbakhsh P, Nakhoda K, Azizi F. (2012) Gender Differences Time Trends for Metabolic Syndrome and Its Components among Tehranian Children and Adolescents. Cholesterol, 2012.
Issam A Mikati
Northwestern University, USA
Title: The use of strain imaging in detection and management of patients with early cardiomyopathy
Time : 13:00-13:30

Biography:
Issam Mikati graduated from the American University of Beirut Medical School. He did Cardiology fellowship at Baylor College of Medicine. He complaeted imaging fellowship at the same institution. He is the associate director of the Echocardiography lab at NorthwesternMemorial hospital in Chicago Illinois. He has published numerous papers in reputed journals and has served as a reviewer of premier journals.
Abstract:
Cardiomyopathy confers a poor prognosis. Early recognition and intervention is key to improve outcome. Classic methods of assessment of LV systolic dysfunction such Left Ventricular Ejection Fraction (LVEF) suffer from wide variance that limits their utility in detection of minor changes in systolic function on serial testing. In addition, the changes in LVEF appear late after significant myocardial damage has occured. This has been shown to affect prognosis of patients. Strain has been shown to be an accurate sensitive marker of LV function with leass varaiance than traditional methods of LV systolic function. It has been shown to drop early in the natural history of many systemic diease that affect the heart such as diabetic cardiomyopathy. Strain shows great promise in management of cardiomyopathies because its efficacy in early detection and potentially effects of treatment.

Biography:
I’m a PhD scholar study in the department of pharmacology and toxicology at Tzu Chi University, our lab is interested in neuropharmacology particular in alcohol effects on the central nerve system and cardiovascular function. My studies focus on the mechanism of acute ethanol intake action on the glutamate signaling within the rostral ventral lateral medulla (RVLM). I have performed the whole animal model with practiced skill in RVLM microinjection of drug and femoral artery surgery for measureing blood pressure, and also have set up the HPLC system to detect the neurotransmitter content. On the other hand, my master's thesis was studied of Amyloid-beta peptides on NMDA receptor activation in rat sympathetic preganglionic neurons using whole cell patch clamp technique. All my training have led me to know more about how the CNS works to control cardiovascular function.
Abstract:
Consumption of ethanol (EtOH) has many effects on physiological functions particular in the central nerve system and cardiovascular system. Hypotension is one of the main features of acute excessive intake of ethanol (alcohol intoxication). In addition, chronic ethanol consumption has been associated with cardiovascular diseases, including hypertension and stroke. The precise mechanisms underlying ethanol regulation of cardiovascular function remains unclear. It is well known central N-Methyl-D-Aspartate (NMDA) receptors are implicated in the modulation of glutamatergic transmission and important in regulating neuronal activity. Recent evidence also suggests that nitric oxide is a key neuromodulator within the central nervous system and its production is associated with NMDA receptor activation. The rostral ventrolateral medulla (RVLM) is known as a vasomotor center, which provides the basal sympathetic outflow and maintains blood pressure (BP). This study was carried out to test the hypothesis that NMDA and NO signalings in the RVLM are involved in the regulation of ethanol-induced changes in BP. The BP response was measured in urethane anesthetized SD rats weighing 280-350 g. EtOH (3.2 g/kg) was applied by intraperitoneal injection (IP). The samples of glutamate and NO were collected by microdialysis every 15 mins in the RVLM and then analyzed with HPLC-ECD and NOx analyzer, respectively. The results showed that IP ethanol elicited a significant increase in the level of glutamate and NO in RVLM and a reduction in BP. Microinjection of ketamine (an NMDA receptor antagonist) or L-NNA (an NOS inhibitor) into the RVLM, which was applied 5 min after administration of EtOH, attenuated EtOH-induced depressor effects. In addition, microinjection of ketamine suppressed the level of NO production. The results suggest that increases in NMDA receptors activation and enhancement of NO synthase activity in the RVLM may play a major role in ethanol-evoked hypotension.

Biography:
Toan’s research is focused on the energetics and mechanisms of the progression from hypertrophy to heart failure, using different techniques of measuring cardiac efficiency: microcalorimetry on trabeculae and respirometry on mitochondrial functions.
Abstract:
An increase in pulmonary arterial pressure increases the load on the right ventricle (RV). With time, progressive pulmonary arterial hypertension (PAH) results in RV hypertrophy, leading ultimately to right-heart failure. In contrast, PAH reduces the passive filling pressure in the left ventricle (LV). This reduces the LV workload, thereby resulting in LV atrophy. Does the structural deformation of the ventricles in right-heart failure affect their mechanoenergetic performance? To address this question, we used the PAH rat induced by a single injection of monocrotaline (MCT) (60 mg/kg) as our experimental model of right-heart failure. Six weeks after MCT injection, the hearts showed signs of right hypertrophy (indexed by increased free wall thickness) and left atrophy. Trabeculae tissue isolated from both ventricles of ‘Control’ and ‘PAH’ rats were mounted in our work-loop calorimeter, and subjected to stress-length work-loops over a wide range of afterloads while contracting at 5 Hz at 37 °C – a protocol designed to mimic the pressure-volume work of the heart. By simultaneously measuring heat production, mechanical efficiency was calculated as the ratio of work output to change of enthalpy (the sum of work and heat). The trabeculae were then required to undergo a preshortening protocol in which isometric force and heat output were measured as functions of muscle length. In right-heart failure secondary to pulmonary hypertension, RV trabeculae show a decrease in myocardial mechanical efficiency correlated with their lower stress-length work performance. The higher activation heat (ordinate of the heat-stress relationship) observed in RV trabeculae from the PAH group reflects an increased energy cost of Ca2+ cycling during contraction. In contrast, LV trabeculae from PAH group sustain normal energy efficiency over a wide range of afterloads.

